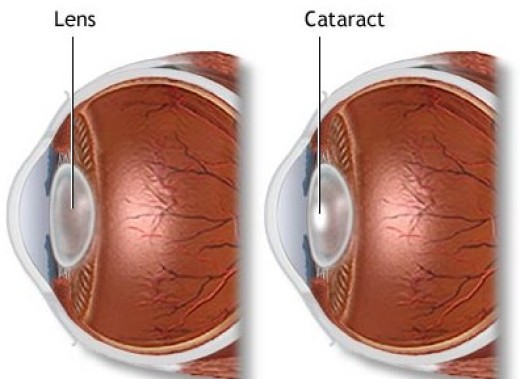
Cataracts occur when the natural clear lens inside the eye, located behind the iris, becomes cloudy over time. This lens is important for focusing light on the back of the eye (the retina) so that images appear clear and without distortion, and the clouding of this lens during cataract formation distorts our vision. Cataracts are usually a very gradual process of normal aging but can occasionally develop rapidly. They commonly affect both eyes, but it is not uncommon for a cataract in one eye to advance more rapidly. Cataracts are very common.
 Precisely why cataracts occur is unknown; however, most cataracts appear to be caused by changes in the protein structures within the lens that occur over many years and cause the lens to become cloudy. Rarely, cataracts can present at birth or in early childhood as a result of hereditary enzyme defects. Severe trauma to the eye, eye surgery, or intraocular inflammation can also cause cataracts to develop more rapidly. Other factors that may lead to development of cataracts at an earlier age include excessive ultraviolet light exposure, diabetes, smoking, or the use of certain medications, such as oral, topical, or inhaled steroids. Other medications that are more weakly associated with cataracts include the long-term use of statins and phenothiazines.
Precisely why cataracts occur is unknown; however, most cataracts appear to be caused by changes in the protein structures within the lens that occur over many years and cause the lens to become cloudy. Rarely, cataracts can present at birth or in early childhood as a result of hereditary enzyme defects. Severe trauma to the eye, eye surgery, or intraocular inflammation can also cause cataracts to develop more rapidly. Other factors that may lead to development of cataracts at an earlier age include excessive ultraviolet light exposure, diabetes, smoking, or the use of certain medications, such as oral, topical, or inhaled steroids. Other medications that are more weakly associated with cataracts include the long-term use of statins and phenothiazines.
Experts have estimated that in the United States, visual disability associated with cataracts accounts for over 8 million physician office visits a year. This number will likely continue to increase as the proportion of people over the age of 60 rises. When people develop cataracts, they begin to have difficulty doing activities they enjoy. Some of the most common complaints include difficulty driving at night, reading, or traveling. These are all activities for which clear vision is essential.
What are the symptoms of cataracts?
Cataract development is often equated to looking through a dirty windshield of a car or smearing grease over the lens of a camera. Cataracts may cause a variety of complaints and visual changes, including blurred vision, difficulty with glare (often with bright sun or automobile headlights while driving at night), dull color vision, increased nearsightedness accompanied by frequent changes in eyeglass prescription, and occasionally double vision in one eye. A change in glasses may help initially once vision begins to change from a cataract; however, as the cataract continues to grow, vision becomes cloudy, and stronger glasses or contact lenses will no longer improve sight.
How are cataracts diagnosed?
Cataracts are detected by the finding of lens opacification during a medical eye examination by an eye-care professional. The abnormal lens can be seen using a variety of specialized viewing instruments. Using a variety of tests, your doctor is able to tell how much a cataract may be affecting your vision. Usual eye tests include testing visual acuity, glare sensitivity, color vision, contrast sensitivity, and a thorough examination of all other parts of the eye. Your doctor will make sure vision loss is not due to other common eye problems, including diabetes, glaucoma, or macular degeneration.
 Most cataracts associated with aging develop slowly, and many patients may not notice visual loss until it is fairly advanced. Despite being told that you have cataracts, it is not imperative to have surgery to remove them until they begin to affect your vision. The development of cataracts is unpredictable; some cataracts remain small and never progress to the point where they affect vision and require treatment, while others progress more quickly. Thus, the decision and timing to proceed with cataract surgery is individualized for each patient. Your doctor will be able to tell you how much of your vision loss is due to cataracts and the type of visual recovery that may be expected if surgery is chosen.
Most cataracts associated with aging develop slowly, and many patients may not notice visual loss until it is fairly advanced. Despite being told that you have cataracts, it is not imperative to have surgery to remove them until they begin to affect your vision. The development of cataracts is unpredictable; some cataracts remain small and never progress to the point where they affect vision and require treatment, while others progress more quickly. Thus, the decision and timing to proceed with cataract surgery is individualized for each patient. Your doctor will be able to tell you how much of your vision loss is due to cataracts and the type of visual recovery that may be expected if surgery is chosen.
Who is a candidate for cataract surgery?
Eye-care professionals may mention during a routine eye exam that you have early cataract development even if you are not yet experiencing visual symptoms. Although your doctor will be able to tell when you first begin to develop cataracts, you will generally be the first person to notice changes in your vision that may require cataract surgery. Clouding of the lens may start to be seen at any age, but it is uncommon before the age of 40. However, a large majority of people will not begin to have symptoms from their cataracts until many years after they begin to develop. Cataracts can be safely observed without treatment until you notice changes in your vision.
Different types of cataract
There are different types of cataract, some of which are due to rare diseases or as a result of local eye injuries or inflammation. However, the two main types are:
- senile (age-related) cataracts – the most common type
- congenital (present at birth) cataracts which are relatively rare but important to diagnose early since vision and ‘seeing’ have to be learnt very early in infancy
Causes of Cataracts
In the UK, most cataracts develop as people get older, and usually they are first noticed around the age of 50-60.
The reason why is not yet known. One theory is that it is caused by a disturbance in the fluids and nutrients in the lens.
In younger people there are certain factors that can increase your risk of getting cataracts. These include:
- Diabetes – this can cause a secondary cataract to develop
- An injury to the eye
- Exposure to ultraviolet light from sunlight
- Medication use such as long-term use of steroid tablets
- Smoking
- Heavy drinking
- A family history of cataracts
Symptoms
- Worsening of the vision -cloudy, fuzzy or filmy vision
- Spots in your vision
- Glare and halos from lights or the sun
- Double vision
- Difficulty in telling the difference between colors, especially shades of blue
- Frequent changes in glasses prescription as eyesight deteriorates
- Second sight – your close-up vision and reading may improve temporarily as the lens changes shape
Different types of cataract surgery in India
There are two types of cataract surgery. Your doctor can explain the differences and help determine which is better for you:
Phacoemulsification or phaco
A small incision is made on the side of the cornea, the clear, dome-shaped surface that covers the front of the eye. Your doctor inserts a tiny probe into the eye. This device emits ultrasound waves that soften and break up the lens so that it can be removed by suction. Most cataract surgery today is done by phacoemulsification, also called “small incision cataract surgery.”
Phacoemulsification is the most modern method of removing a cataract lens. This surgery is done under topical anaesthesia and no stitches are applied. This greatly reduces trauma to the eye.
Extracapsular surgery
Your doctor makes a longer incision on the side of the cornea and removes the cloudy core of the lens in one piece. The rest of the lens is removed by suction. After the natural lens has been removed, it often is replaced by an artificial lens, called an intraocular lens (IOL). An IOL is a clear, plastic lens that requires no care and becomes a permanent part of your eye. Light is focused clearly by the IOL onto the retina, improving your vision. You will not feel or see the new lens.
The Ophthalmology Department at Apollo Hospitals offers expert surgical and non-surgical management of eye ailments using the most superior technology available.
They are a specialized hand at Phaco Surgery rendered to cure cataracts.
- Lasik Laser
- Lacrimal Apparatus
- Yag Laser
- Occular Topograph
- Coherent Argon Laser Topcon Fundus Camera
- A-scan Biometer
- 3mm Auto Refractometer
- Canon Wall mount Welch Allyn Ophthalmoscope
- Retinoscope Carl
- Zena KPM Perimeter Keratometer
- Shin Nippon Indirect Ophthalmoscope
- Visual Field Analyser
- Hiene Contact lens service